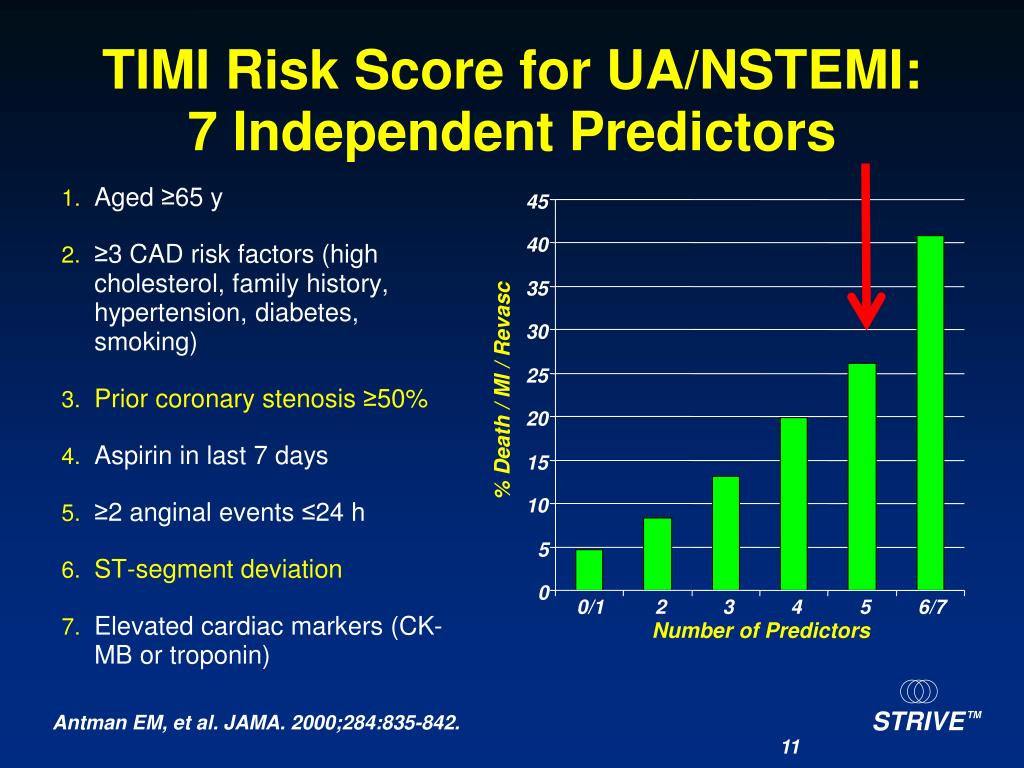
Though no score is perfect, risk scores are still considered as valuable tools in clinical decision-making. Based on clinical parameters, multiple risk scores have been developed to aid physicians in risk stratification in complement to clinical judgement. For every ACS patient, a risk assessment is performed prior to treatment decision-making at different points along the ACS pathway. 2009 4(11):e7947.Acute coronary syndrome (ACS), including unstable angina (UA), non-ST-segment elevation myocardial infarction (NSTEMI) and ST-segment elevation myocardial infarction (STEMI), is one of the most frequent reasons for cardiac hospital admission. Does simplicity compromise accuracy in ACS risk prediction? A retrospective analysis of the TIMI and GRACE risk scores. Īragam KG, Tamhane UU, Kline-Rogers E, et al. 2015 ESC Guidelines for the management of acute coronary syndromes in patients presenting without persistent ST-segment elevation. Prediction of risk of death and myocardial infarction in the six months after presentation with acute coronary syndrome: prospective multinational observational study (GRACE) BMJ. Global Registry of Acute Coronary Events Investigators Predictors of hospital mortality in the Global Registry of Acute Coronary Events. Granger CB, Goldberg RJ, Dabbous O, et al. The TIMI risk score for unstable angina/non-ST elevation MI: a method for prognostication and therapeutic decision making. GRACE risk score NSTE-ACS NT-proBNP TIMI risk score myocardial infarction.Īntman EM, Cohen M, Bernink PJ, et al. However, incremental prognostic value of NT-proBNP beyond the GRACE risk score could not be demonstrated. In patients with NSTE-ACS, NT-proBNP and the GRACE risk score (but not the TIMI risk score) both have good and comparable predictive value for 30-day mortality. Adjustment of the GRACE risk score by adding NT-proBNP did not improve prognostication: AUC 0.86 ( p=0.57), integrated discrimination improvement 0.04 ( p=0.003), net reclassification improvement 0.12 ( p=0.21). The predictive value of NT-proBNP did not differ significantly compared to the GRACE risk score (area under the curve ) 0.85 vs 0.87 p=0.67) but was considerably higher in comparison to the TIMI risk score (AUC 0.60 p<0.001). On logistic regression analysis NT-proBNP and the GRACE risk score (but not the TIMI risk score) both independently predicted mortality at 30 days. We compared the predictive value of NT-proBNP to both risk scores and evaluated whether NT-proBNP improves prognostication by using receiver operator curves and measures of discrimination improvement.Ī total of 1324 patients were included and 50 patients died during follow-up. NT-proBNP levels on admission were measured and the GRACE and TIMI risk scores were assessed. Patients included in our ACS registry were candidates. To evaluate the predictive value of NT-proBNP for 30-day mortality over and beyond the Global Registry of Acute Coronary Events (GRACE) and Thrombolysis In Myocardial Infarction (TIMI) risk scores in patients with NSTE-ACS. Whether NT-proBNP has incremental prognostic value beyond established risk strategies is still questionable. The biomarker N-terminal pro-brain natriuretic peptide (NT-proBNP) predicts outcome in patients with non-ST-elevation acute coronary syndromes (NSTE-ACS).
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
